Created as Elon prepared to welcome its inaugural cohort of nursing students, the center will offer an array of capabilities and training to over 250 students in the School of Health Sciences.

Elon University has opened a new Interprofessional Simulation Center that will serve as an experiential health care learning hub and support over 250 students in the School of Health Sciences. The center was completed in May and as the university prepares to welcome its inaugural cohort of nursing students, members of the university community saw all it is capable of during an open house on Wednesday, Aug. 18.
“My professional goal is to provide a space for students to come and practice their hands-on skills,” said Nita Skillman, director of interprofessional simulation at Elon.
The state-of-the-art Interprofessional Simulation Center is located on the second floor of the Gerald L. Francis Center. It’s equipped with multiple beds and designed to provide students will the ability to practice health care techniques on high- and low-fidelity manikins, standardized patients and clients from the local community using “superior” recording equipment in a variety of settings.
Skillman said two main objectives she has are to create students who have excellent patient-centered communication and who are known for being team players in health care. The Interprofessional Simulation Center was created to prepare for the incoming cohort of students within the newly created Nursing Program, a significant and early achievement detailed in the Boldly Elon strategic plan for 2030.
Spread across two main spaces in the Francis Center, the center includes the clinical skills lab and the simulation lab. The clinical skills lab has seven beds separated by curtains and houses most of the manikins. The manikins vary in age from infants to adults and are provide numerous capabilities, such as childbirth.
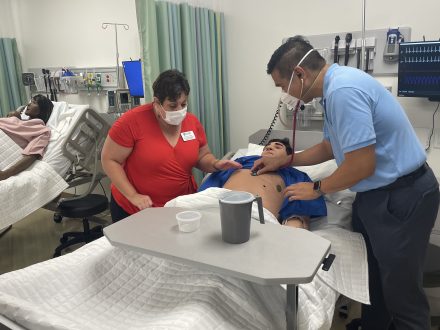
“That lab space is built to look like a hospital ward,” Skillman said. “We’re about developing the muscle memory now in that lab so there’s no surprises when they walk on a clinic floor.”
The simulation lab has a pre-briefing and debriefing period. During the pre-briefing, the student is told of what situations they will encounter during the simulation and remind them to suspend their disbelief.
“As much as we work to make simulation as real life as possible, there’s always going to be the one off that just doesn’t quite match,” Skillman said.
The debrief period occurs after the simulation and students will sit down with someone from the staff of certified health care simulation educators to review how they did. Students will be recorded during the simulation and scored on a rubric depending on the services they performed during the simulation.
“Also, the debriefing is a chance for the student to decompress from that potentially stressful testing situation,” Skillman said.
Another important element of the debriefing process is the faculty will allow for the student to do more of the talking, as opposed to just reading off each wrong decision the student made.
“The purpose of debriefing is to truly think out loud what steps you took, maybe what you would do differently and what were you missing going into the room,” Skillman said.
In the simulation lab, there’s a home health care open concept area comprised of a kitchenette, small living room and small bedroom. This area is dedicated to preparing students for working in a patient’s home.

Surrounding the home health care area are seven clinical rooms, five of them are standard clinic rooms, one is set up to resemble an ICU room and the other is a hospital room.
“Everything we do on this floor is interprofessional. Whether you’re a nurse, a physician assistant or a physical therapist, all equipment you need for that profession are in those rooms,” Skillman said.
The simulation can last anywhere from five minutes to five hours, Skillman said, and depends upon what the student is working on.
“If we’re running a blood draw, it doesn’t take you very long to stick an arm and pull blood,” she said. “However, it’s going to take you a little bit longer to deliver a baby.”
Skillman stressed that the Interprofessional Simulation Center is a “safe place” where students are allowed to make mistakes and take the time to thoroughly learn from them so that when they find themselves providing care in the real world, they are more than prepared.
“Basically, we are psychologically preparing the students for success,” Skillman said. “When our students are psychologically prepared when they enter the door, they view that door no differently than if they were walking into a hospital clinic.”



